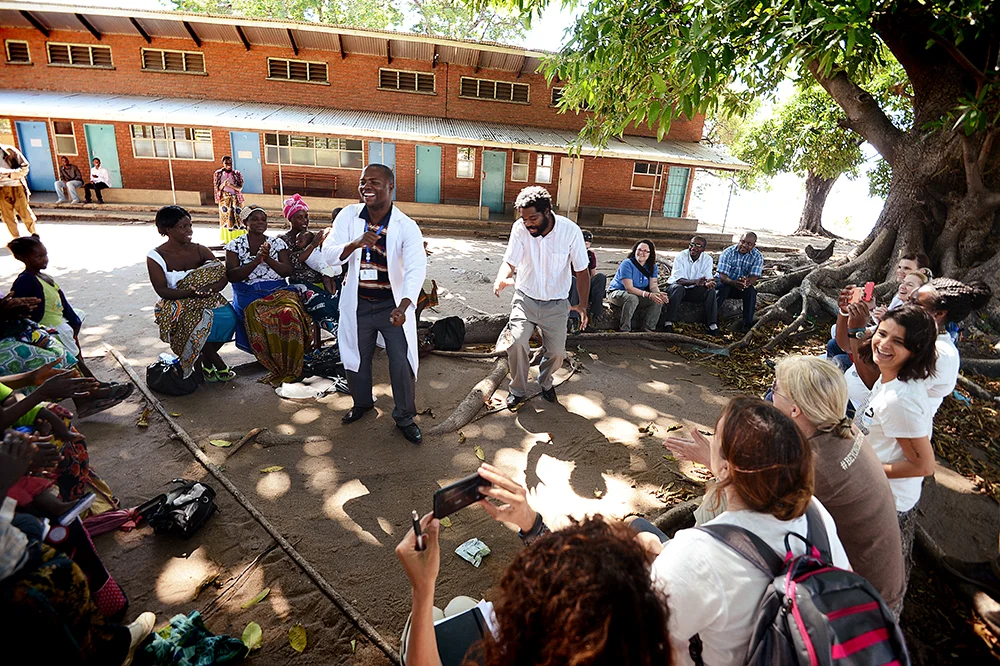malawi: health care
Monkey Bay Community Hospital
On Day 2 of our trip to Malawi, my travel companions and I visited two health care facilities. I'm not going to lie: whenever I do these trips, visiting clinics is my least favourite thing to do -- it's tough seeing people, especially children, who are ailing. And I was particularly nervous about this trip, since health statistics for Malawi are bleak: life expectancy in Malawi is one of the lowest in the world, at 60 years, owing primarily to the rapid spread of HIV/AIDS, but also malaria, tuberculosis, and malnutrition. Preventable causes such as malaria, diarrhea, pneumonia, anemia, malnutrition and neonatal complications constitute 70% of child deaths. Making things worse, poor health is exacerbated by Malawi's land-locked geography, rendering health care services and safe drinking water and sanitation scarcely accessible. There are few hospitals, clinics, doctors, nurses or health care workers, with only 1.9 physicians available for every 100,000 people. And of course, with only 9% of the residents of Malawi having access to electricity, the hospitals and clinics are often at the mercy of the already overtaxed power grid as well.
But there is good news.
Thanks to The Global Fund, an international financing organization which aims to fight, prevent and treat tuberculosis, malaria and HIV/AIDS, Malawi has received nearly $900 million since 2003 to fight disease and strengthen health systems. The Global Fund has administered nearly 7 million bed nets in Malawi to prevent malaria, in addition to securing Anti-retroviral Therapy (ART) for 420,000 infected by the AIDS virus. In addition, through the US President's Emergency Plan for AIDS Relief (PEPFAR), a USAID-implemented program launched in 2006 in Malawi, in 2014 alone USAID provided testing for more than 1.1 million Malawians, including more than 350,000 pregnant women. USAID started 62,000 HIV-positive patients on ART, including 27,000 pregnant women, and kept 217,000 HIV-positive patients on ART at USAID-supported health facilities.
There is, of course, a lot of work to do: with the clinics often overcrowded (requiring patients to share beds, sometimes), medicine shortages and frequent power outages, there's still a long way to go. But despite this, everywhere we turned, we saw dedication and hope. And dedication and hope, my friends, can go very far.
This is Christopher Kandionamaso, a nurse and programme director at the health care facilities we visited, who gave us our tour. Great guy.
After our tour of Monkey Bay Community Hospital, we visited the more remote Nkope Health Centre, where a group of HIV-positive mothers sat with us at the foot of a huge tree to share their stories. They included incredible hardships, of course (including have to walk many kilometers simply to be treated), but also stories of gratitude, that they were getting good care, the medicines they needed, and often their children were born HIV-negative. We were all quite moved at how open they were with their stories.
As our meeting wound down, Christopher stood and said, "whenever we have meetings, we always close with a song. Do you have a song you'd like to share with us?" he asked, as we stared back at him with blank faces.
"No?" And then he looked around at the Malawian mothers, and just broke into song.
Without skipping a beat, the women began singing with him, call-and-answer, in perfect harmony, while clapping along. It was beautiful.
And then suddenly, Christopher's project manager jumped right in the middle of the circle, and started freestyling.
Well, naturally, our group wasn't going to take that sitting down. And so dance we did!
(I've said it before and I'll say it again: we don't sing and dance enough in our meetings in the west. This is probably especially true at our hospitals: imagine how much better we'd all feel!)
The truth is, singing, dancing and joy were a big part of our trip to Malawi.
But that's a story for tomorrow's post.
Song: Totoumo vy Diabel Cissokho & Ramon Goose
Have you joined ONE Girls & Women yet? You should -- you'll get many more stories like this one, as well as ways you can help -- and the best part? ONE will never ask for your money -- just your voice. Click here to like the ONE Girls & Women Facebook page, and/or the image below to join!